Enhancing intraoperative visibility and postoperative safety through standardized radiopaque marker integration
Introduction
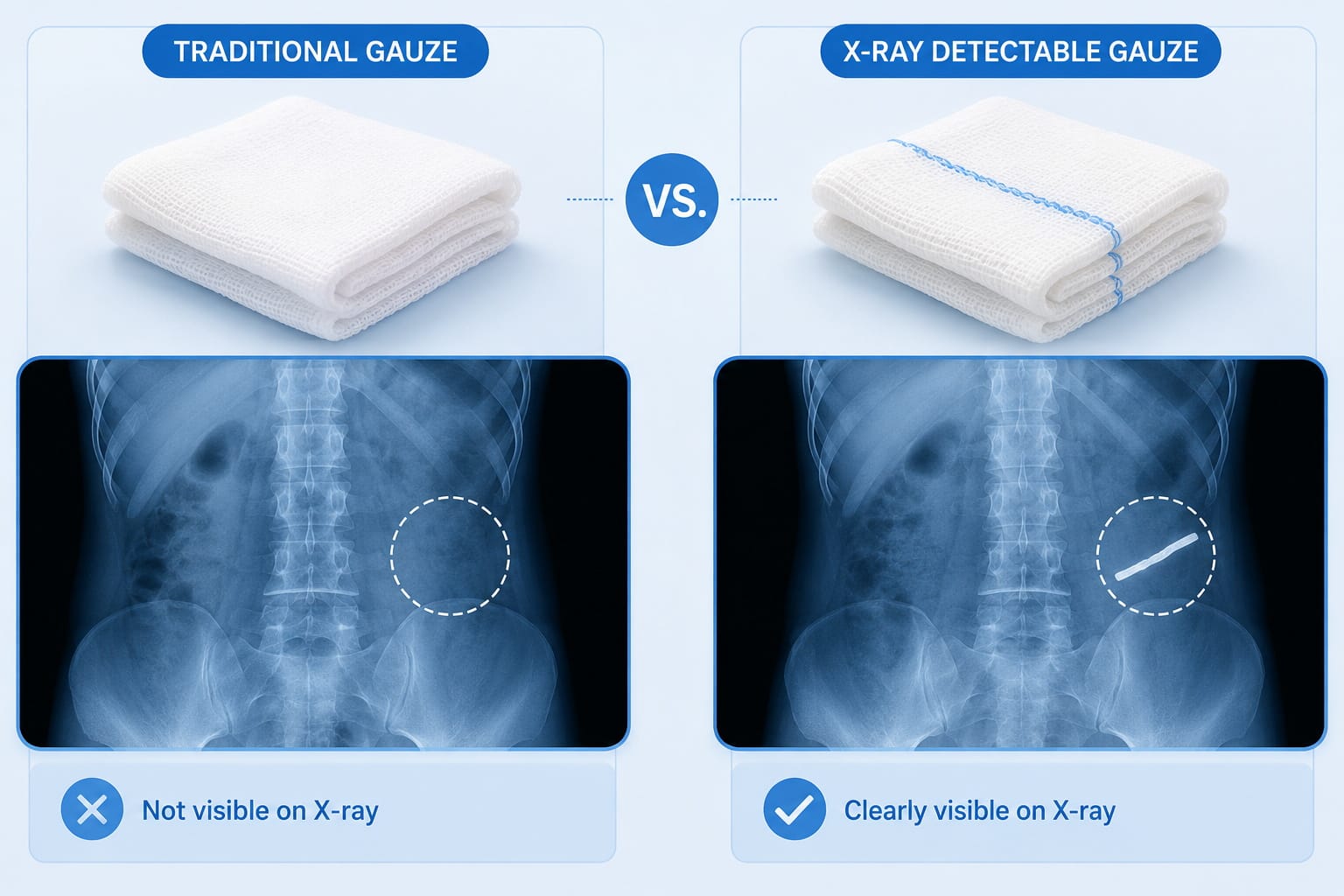
X-ray Detectable Gauze is a critical category of surgical consumables designed to improve intraoperative safety and postoperative outcomes. By incorporating radiopaque markers—typically barium sulfate-impregnated threads or strips—these gauze products can be detected using X-ray imaging, addressing a key risk in surgical procedures: retained surgical items (RSIs). With increasing emphasis on patient safety and regulatory compliance, X-ray Detectable Gauze has become a standard requirement in modern operating rooms.
I. Intraoperative Detection and Prevention of Retained Surgical Items
One of the primary functions of X-ray Detectable Gauze is to prevent RSIs, a serious and preventable surgical complication. According to guidelines from the Association of periOperative Registered Nurses (AORN) and multiple clinical studies published between 2022–2025, retained gauze accounts for a significant proportion of surgical sentinel events.
Radiopaque markers embedded in the gauze enable rapid identification under X-ray imaging when surgical counts are inconclusive. This is particularly critical in emergency surgeries, high-blood-loss procedures, or complex operations involving multiple teams. By providing a secondary verification method beyond manual counting, X-ray Detectable Gauze significantly reduces medico-legal risks and improves patient safety outcomes.
II. Compliance with International Surgical Safety Standards
X-ray Detectable Gauze is not merely a recommended product but is increasingly mandated by clinical guidelines and hospital accreditation systems. For example, surgical practice standards outlined in operating room nursing protocols explicitly require the use of detectable surgical dressings within surgical cavities.
From a regulatory perspective, organizations such as The Joint Commission emphasize the importance of RSI prevention strategies, including the use of detectable surgical materials. Hospitals that fail to adopt such measures may face compliance issues, increased liability, and reputational risks. Therefore, X-ray Detectable Gauze plays a crucial role in aligning surgical practices with global safety standards.
III. Enhanced Workflow Efficiency in Surgical Teams
Beyond safety, X-ray Detectable Gauze contributes to improved workflow efficiency in the operating room. In situations where discrepancies arise during surgical counts, the availability of X-ray detection reduces the need for prolonged manual searches, minimizing anesthesia time and associated risks.
Modern surgical environments increasingly integrate imaging verification protocols. X-ray Detectable Gauze seamlessly fits into these workflows, allowing surgical teams to quickly confirm the absence of retained materials without disrupting procedural flow. This is particularly valuable in high-throughput surgical centers where efficiency and accuracy must coexist.
IV. Material Design and Clinical Performance Advantages
X-ray Detectable Gauze is engineered to maintain all functional properties of traditional gauze—such as high absorbency, softness, and biocompatibility—while adding radiographic visibility. The radiopaque threads are designed to be clearly visible under imaging without compromising the flexibility or usability of the gauze.
Recent innovations have focused on improving marker contrast, durability, and integration techniques to prevent marker detachment. High-quality X-ray Detectable Gauze ensures consistent detectability even after prolonged exposure to bodily fluids, which is essential for maintaining reliability during lengthy procedures.

V. Application Scenarios Across Surgical Specialties
X-ray Detectable Gauze is widely used across multiple surgical disciplines, including general surgery, neurosurgery, abdominal surgery, and trauma care. It is especially critical in procedures involving deep cavities, such as laparotomies or thoracic surgeries, where visibility is limited.
In neurosurgical applications, smaller X-ray detectable cottonoids are used to protect delicate tissues while ensuring traceability. In abdominal surgeries, larger X-ray detectable laparotomy sponges are employed for fluid absorption and organ retraction. These diverse applications highlight the adaptability and necessity of X-ray Detectable Gauze across clinical settings.
Conclusion
X-ray Detectable Gauze serves as a vital safeguard in modern surgical practice by combining traditional wound management functions with advanced imaging detectability. Its role in preventing retained surgical items, ensuring compliance with international safety standards, enhancing workflow efficiency, and supporting diverse surgical applications makes it indispensable in contemporary healthcare systems. As patient safety continues to be a central focus, the adoption of X-ray Detectable Gauze is expected to further expand, ultimately contributing to higher standards of surgical care and risk management.