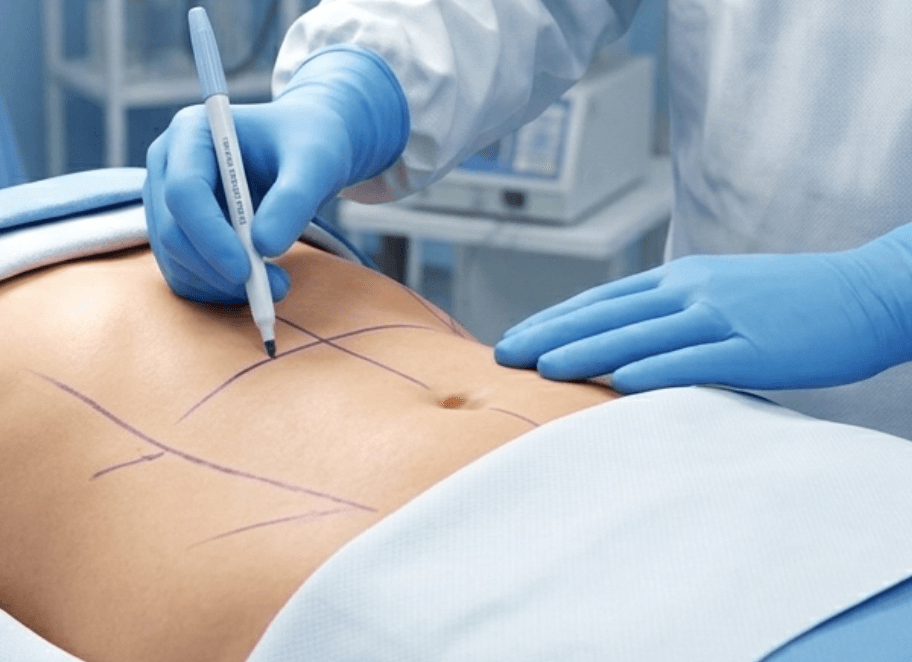
A comprehensive overview of medical-grade skin marking pens in preoperative planning, procedural accuracy, and product selection for clinical use
Overview of Surgical Skin Markers in Clinical Practice
Surgical skin markers are essential single-use medical devices designed for precise marking on the skin surface prior to surgical or interventional procedures. These markers utilize biocompatible, non-toxic ink that is resistant to antiseptic solutions such as chlorhexidine and povidone-iodine, ensuring visibility throughout the procedure. According to recent clinical guidelines and infection control standards (e.g., AORN and CDC recommendations), the use of sterile, single-use skin markers reduces cross-contamination risks and enhances procedural safety.
In modern healthcare environments, skin markers are widely used across operating rooms, outpatient clinics, and aesthetic medicine settings. Their role extends beyond simple marking—they contribute directly to surgical accuracy, patient safety, and workflow efficiency.
Clinical Application Scenarios of Skin Markers
Preoperative Site Marking and Surgical Planning
Skin markers are most commonly used in preoperative settings to identify incision sites, anatomical landmarks, and surgical boundaries. This is particularly critical in procedures requiring high precision, such as plastic surgery, orthopedic surgery, and neurosurgery. Proper marking supports compliance with protocols like the Universal Protocol for Preventing Wrong Site Surgery.
Markers with fine tips enable surgeons to create detailed outlines, while maintaining clarity even after skin preparation. Studies have shown that accurate preoperative marking can significantly reduce surgical errors and improve intraoperative efficiency.
Interventional Procedures and Radiology Guidance
In interventional radiology and minimally invasive procedures, skin markers are used to indicate entry points for needles, catheters, or imaging alignment. For example, during CT-guided biopsies or ultrasound-guided injections, precise marking ensures correct targeting and reduces procedural time.
Markers used in these settings must provide high contrast visibility and quick-drying properties to prevent smudging. Additionally, compatibility with imaging modalities (non-artifact causing) is essential.
Dermatology and Aesthetic Medicine Applications
In dermatology and cosmetic procedures, skin markers are used to outline treatment areas for laser therapy, botulinum toxin injections, dermal fillers, and lesion excisions. Fine-tip markers allow practitioners to map facial symmetry and injection points with high precision.
For aesthetic applications, ink visibility and ease of removal post-procedure are important considerations. Some markers are designed with dual tips—one for marking and one for gentle removal or correction.
Emergency and Bedside Procedures
Skin markers are also utilized in emergency departments and bedside procedures such as thoracentesis, central line placement, or wound management. In these fast-paced environments, markers must be reliable, easy to use, and capable of writing on moist or irregular skin surfaces.
Single-use sterile packaging is particularly important in these scenarios to maintain infection control standards.
Key Challenges and Clinical Needs
Despite their simplicity, selecting an appropriate skin marker involves addressing several clinical pain points:
- Ink Persistence vs. Removability: Ink must resist disinfectants but still be removable post-procedure without skin irritation.
- Sterility Assurance: Non-sterile markers pose infection risks, especially in invasive procedures.
- Tip Precision: Different procedures require varying tip sizes (fine vs. regular).
- Allergen Safety: Ink composition must be hypoallergenic and compliant with medical-grade standards.
Addressing these challenges is essential for improving both clinician experience and patient outcomes.
Product Selection Criteria and Recommendations
When choosing a surgical skin marker, healthcare providers should consider the following factors:
- Sterility: Prefer EO-sterilized, individually packaged markers for surgical use.
- Ink Quality: Medical-grade, gentian violet-based or equivalent ink that is non-toxic and antimicrobial.
- Tip Design: Fine tip for detailed marking; regular tip for general use. Dual-tip options offer versatility.
- Drying Time: Quick-drying ink reduces smearing risk.
- Resistance: Ink should withstand alcohol-based and iodine-based skin prep solutions.
- Ease of Removal: Especially important in dermatology and aesthetic procedures.
For hospitals and surgical centers, standardized procurement of high-quality disposable skin markers can streamline workflows and ensure compliance with infection control protocols. For distributors and suppliers, offering a range of marker types (sterile/non-sterile, single/double tip) can meet diverse clinical demands.